Remembering Our Veterans
Today is Memorial Day in the US, when we remember those who gave their lives in service of their country. I had an uncle, Jim Morrow, who died in Vietnam, on October 15, 1967. His name is inscribed on the Vietnam Memorial wall in Washington DC. Those we remember are those who willingly joined the service as career veterans, or were called to active service in a time of war.

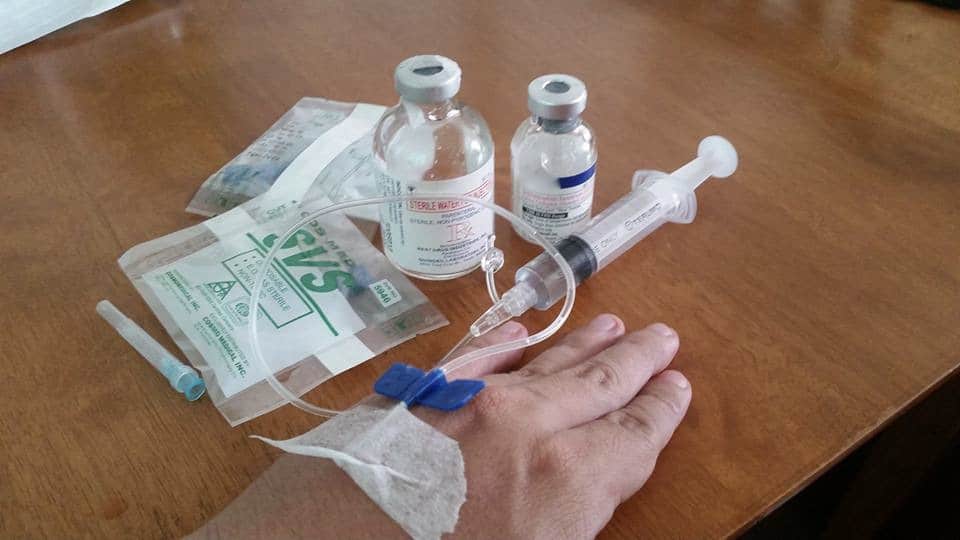
I often think of our bleeding disorder community on Memorial Day. We were at war at one time, from the late 1970s through the 1980s, fighting the scourge of HIV. My son with hemophilia was born in 1987, at the height of the HIV battle. The Ray brothers had just been bombed out of their home in Florida. Our “soldiers” were gathering for a battle against pharma and the US government, to hold them accountable for the contamination of our nation’s blood supply. It was a scary time, especially for a new parent. I attended my first NHF meeting in 1992, and witnessed so much hostility and anger, directed at the displays by pharma, and at each other. Some of our community members were taking a legal approach, hoping for compensation through negotiation; others wanted a more militant approach to solving the accountability problem. So many had died. So many.
I was on the “other” side; my baby had escaped the dreaded HIV infection by only a year or two. When I met these leaders and soldiers in the community, I was struck by their dedication, knowledge and courage. Some were dying already, but fought the good fight to win compensation for all. That would be our only freedom. They were victims of this insidious infection, but became soldiers to defend us, the ones who barely escaped. Their efforts ensured a safer future for all.
Many of those soldiers have died now, but I still remember them. I feel honored to have known them. And I always appreciate how by fate, my child escaped their fate by mere months. I keep photos of some of them on a shelf at home, and have for the past 20 years. Names like Michael Davon and Tom Fahey, co-founders of the Committee of Ten Thousand (COTT); Dave Madeiros, a visionary leader who sought to provide funds to the community by owning a specialty pharmacy—his insights into insurance changes and prophecy about managed care and restrictions all came true.
And some photos are of patients who died, who inspire me all the time. It’s important we remember them all, and carry on their legacy. We are of a new generation now, and our community may be forgetting these veterans.

How can you get to know them and remember them? Read And the Band Played On (also an HBO movie). Watch the movie “Bad Blood: A Cautionary Tale.” Buy the book Dying in Vein. If you have hemophilia, or a child with it, knowing your community history is every bit as important as knowing American history this Memorial Day.